Read
From Our Care Team
Clinical resources, and health & wellness advice

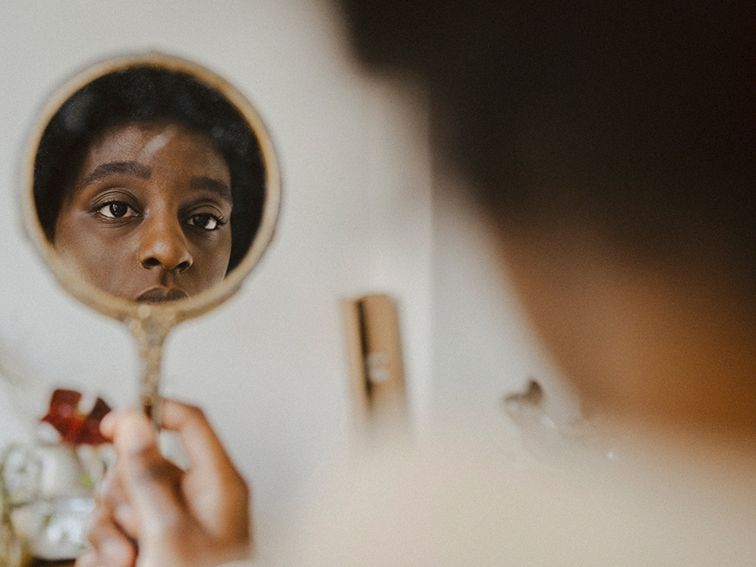
Featured
I'm not stressed. Am I? Oh no.
When you have a lot of stress in your life, it can start to feel normal. You may not even notice your clenched jaw or racing mind. To help you reset, see what Firefly providers had to say about stress in their own lives.

April 30, 2024
Bringing care into the home for an expecting mom
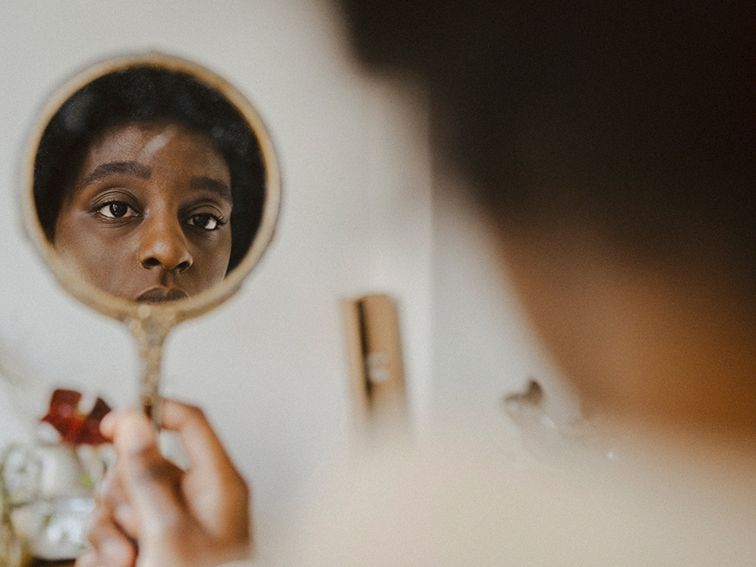
April 1, 2024
I'm not stressed. Am I? Oh no.

April 1, 2024
The Many Health Benefits of Fiber

October 16, 2024
Taking control of asthma and healthcare costs

March 22, 2023
Colorectal Cancer Q&A

October 10, 2023
Breast Cancer Q&A

March 30, 2023
New to fatherhood and virtual care

March 23, 2022
Celebrating a World of Flavors

February 21, 2022
Racial and Ethnic Disparities in Blood Pressure Treatment for African Americans

September 2, 2021
How Much Alcohol is Safe?

August 15, 2022
How Much Water Do You Need?

August 10, 2022
Hold the Salt. Or the Sodium? Both.